The global coronavirus pandemic has strained the health care system in Illinois and the United States more broadly.
Many states saw declines in COVID-19 positive case rates and hospitalizations in late April and early June. COVID-19 cases and hospitalizations, however, have surged since states began lifting certain restrictions on economic activity and mobility. Arizona, Texas, and Florida are all facing hospital capacity concerns. The State of Washington has required face masks after Yakima County ran out of hospital beds to help battle the virus. California has reinstated some restrictions on indoor activities and businesses – such as closing bars, indoor eating at restaurants, gyms, movie theaters, and more.
Illinois has recently fared much better in combating the virus. In fact, the University of Chicago Medical Center is eliminating units dedicated to COVID-19 patients as the number of people with the illness has dropped. Illinois is also one of 17 states that is currently meeting minimum testing targets to mitigate the spread of the virus. The state has a 3% seven-day statewide positivity rate.
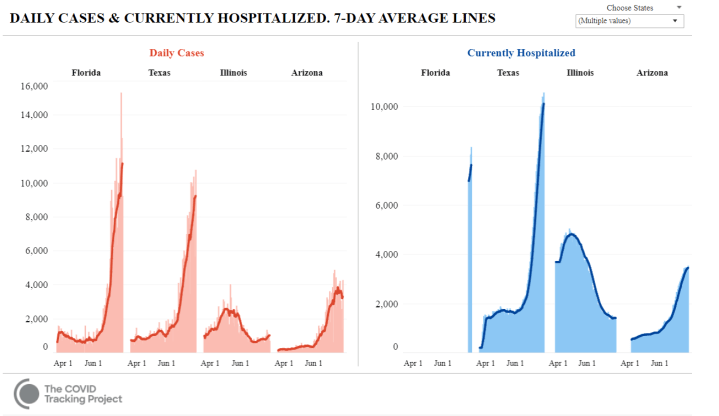
Nevertheless, Illinois remains one of the states that was hit hardest by the outbreak, with more than 155,000 cases and more than 7,200 deaths as of July 14. In April and May, many Illinois hospitals were overwhelmed with an influx of COVID-19 patients. And, in general, Illinois’ unionized hospitals were better prepared for the pandemic in terms of staffing levels, according to a new report from the Illinois Economic Policy Institute (ILEPI). That’s because union hospitals had significantly lower nurse turnover rates, have fewer nurse vacancies, and have more infection prevention and control personnel coming into the pandemic.

In addition, registered nurses at union hospitals in Illinois are able to devote 1 to 4 more hours of care to individual patients, on average, which can mean life or death for gravely ill patients. In Chicago, unionized hospitals had better staffing levels than nonunion hospitals, which may have reduced COVID-19 mortality rates (although more Chicago-specific research is needed to know for sure). Finally, recent economic research has found that union hospitals outperform nonunion hospitals in 12 out of 13 (92%) patient-sensitive outcomes, including hospital-acquired pneumonia and in-hospital deaths– which are particularly important during COVID-19.
While many hospitals are struggling financially due to a dramatic 50%-70% decrease in elective surgeries, the federal government allocated $175 billion in relief funds to hospitals and health care providers through the CARES Act and other measures. According to the Centers for Disease Control and Prevention (CDC), Illinois hospitals received at least $1.1 billion in federal subsidies, with large nonunion hospitals receiving more federal assistance ($30,000 per bed) than large union hospitals ($26,000 per bed).

Of course, further research is needed to assess the performance of Illinois’ hospitals during the COVID-19 pandemic. This includes whether unionized hospitals had better outcomes than nonunion hospitals, particularly in Cook County which was hit hardest by the virus. However, prior to the pandemic, the data suggests that unionized hospitals were generally better prepared for the public health crisis because nurses’ unions enhance staffing levels, boost nurse retention rates, and improve patient care.
Please wear a mask or face covering in public, practice social distancing, wash your hands regularly, and stay safe while we continue to combat COVID-19.

